Exploring the Complexity of Psoriasis Mechanism
Psoriasis is a chronic autoimmune skin condition that affects millions of people worldwide. Understanding the mechanism behind psoriasis is crucial for developing effective treatments and improving the quality of life for individuals living with this condition.
What is Psoriasis?
Psoriasis is a non-contagious skin disorder characterized by the rapid buildup of skin cells. It presents as raised, red patches covered with silvery scales, which can be itchy and painful. Common areas affected include the elbows, knees, scalp, and lower back. Psoriasis can vary in severity from mild to severe and can have a significant impact on an individual’s physical and emotional well-being.
Psoriasis Mechanism
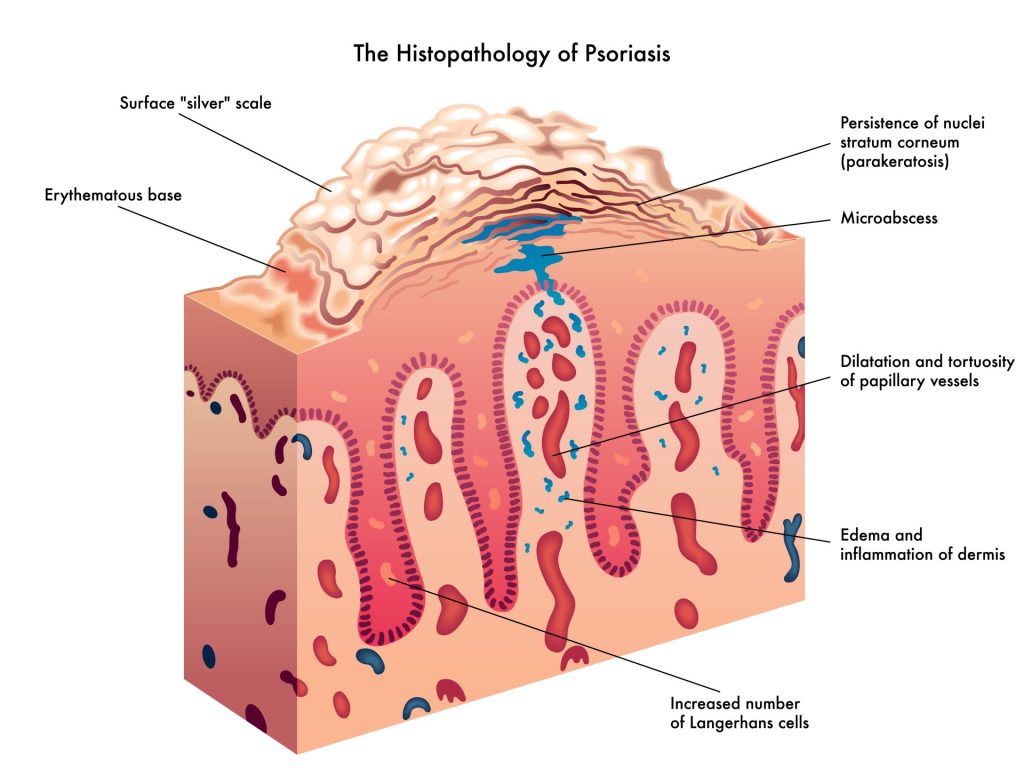
Understanding the Immune System
To comprehend the psoriasis mechanism, it’s important to first understand the role of the immune system. The immune system serves as the body’s defense mechanism, protecting it against harmful substances and invading pathogens. It consists of a complex network of cells, tissues, and organs working together to maintain health.
The Role of Genetics
While the exact cause of psoriasis remains unknown, genetics play a significant role in its development. People with a family history of psoriasis are more likely to develop the condition themselves. Specific genes related to the immune system and skin cell growth have been identified as potential contributors to psoriasis susceptibility.
Inflammation and Psoriasis
Inflammation is a key component of the psoriasis mechanism. In individuals with psoriasis, the immune system mistakenly identifies healthy skin cells as foreign substances, triggering an immune response. Inflammatory cytokines, such as tumor necrosis factor-alpha (TNF-alpha) and interleukins, are released, leading to inflammation and the characteristic symptoms of psoriasis.
Psoriasis Triggers
Psoriasis can be triggered or aggravated by various factors, including environmental influences and lifestyle choices. Common psoriasis triggers include stress, infections, certain medications, smoking, and excessive alcohol consumption. Identifying and avoiding these triggers can help manage psoriasis symptoms and reduce flare-ups.
The Role of T Cells
T cells, a type of white blood cell, play a crucial role in the development of psoriasis. In individuals with psoriasis, T cells become overactive, leading to increased production of inflammatory cytokines. These activated T cells migrate to the skin, where they promote inflammation and stimulate the excessive growth of skin cells.
The Psoriasis Cycle
The psoriasis cycle refers to the continuous process of skin cell turnover that occurs in psoriasis-affected individuals. Normally, skin cells take about a month to mature and shed. However, in psoriasis, this process is significantly accelerated, with skin cells maturing and shedding in a matter of days. The rapid turnover results in a buildup of thickened, scaly skin patches.
Immune System Dysregulation
Psoriasis is characterized by immune system dysregulation, wherein the immune response is abnormally activated. Multiple cell signaling pathways, such as the Janus kinase/signal transducer and activator of transcription (JAK/STAT) pathway and the nuclear factor kappa B (NF-kB) pathway, are dysregulated in psoriasis. These abnormalities contribute to the chronic inflammation and abnormal skin cell growth observed in psoriasis lesions.
Targeted Therapies
In recent years, targeted therapies have revolutionized the treatment of psoriasis. Biologic medications, such as tumor necrosis factor inhibitors and interleukin inhibitors, target specific immune system components or inflammatory pathways involved in psoriasis. By blocking these specific targets, these medications can effectively reduce inflammation and alleviate psoriasis symptoms.
Topical Treatments
Topical treatments are commonly used for mild to moderate psoriasis. They are applied directly to the skin and come in various forms, including creams, ointments, and gels. Topical treatments may contain corticosteroids, vitamin D analogs, salicylic acid, or coal tar. They work by reducing inflammation, slowing down skin cell growth, and moisturizing the skin.
Phototherapy and Psoriasis
Phototherapy, also known as light therapy, is a treatment option for moderate to severe psoriasis. It involves exposing the skin to controlled doses of ultraviolet (UV) light, either in a medical setting or using specialized equipment at home. UV light slows down skin cell growth and reduces inflammation, leading to improved psoriasis symptoms.
Lifestyle and Psoriasis Management
While there is no cure for psoriasis, certain lifestyle modifications can help manage the condition effectively. Maintaining a healthy lifestyle with regular exercise, a balanced diet, and stress management can contribute to overall well-being and potentially reduce psoriasis flare-ups. It’s also important to identify personal triggers, such as specific foods or activities, and avoid them whenever possible.
Psychological Impact of Psoriasis
Psoriasis not only affects physical health but also has a profound psychological impact on individuals living with the condition. The visible symptoms and chronic nature of psoriasis can lead to feelings of self-consciousness, embarrassment, and low self-esteem. It is crucial to address the emotional and psychological aspects of psoriasis, seeking support from healthcare professionals, support groups, or therapy if needed.
Future Research and Potential Breakthroughs
Ongoing research is focused on unraveling the complexities of the psoriasis mechanism and identifying new treatment approaches. Promising areas of research include exploring novel targets within the immune system, investigating the gut-skin axis, and developing advanced gene therapies. Continued advancements in understanding the psoriasis mechanism hold the potential for more effective and personalized treatment options in the future.
Conclusion
Understanding the mechanism behind psoriasis is essential for developing effective treatments and improving the lives of individuals affected by this chronic condition. By exploring the role of the immune system, genetics, inflammation, and other contributing factors, researchers and healthcare professionals are continually working towards better management and potential cures for psoriasis.
Reference:
- Frank O. Nestle, Curdin Conrad, Mechanisms of psoriasis, Drug Discovery Today: Disease Mechanisms, Volume 1, Issue 3, 2004, Pages 315-319, ISSN 1740-6765, https://doi.org/10.1016/j.ddmec.2004.11.005 (https://www.sciencedirect.com/science/article/pii/S1740676504000586) Abstract: Psoriasis is a polygenic, chronic relapsing inflammatory autoimmune disease based on an interplay between antigen-presenting dendritic cells, T cells and keratinocytes creating the typical signature skin lesions, that is sharply demarcated reddish and scaly plaques. The discovery of master cytokines (e.g. TNF-α) and master cells (e.g. dendritic cells and T cells) in combination with new humanized animal models will lead to rationale drug development for the benefit of patients suffering from this as yet incurable disease.
- https://www.psoriasistreatmentbangalore.com/psoriasis-symptoms-types-and-treatment/

