Ear Psoriasis Treatment: A Complete Guide to Managing, Healing, and Reclaiming Your Life
Ear psoriasis treatment is one of the most searched yet least discussed topics in dermatological care. If you’ve ever dealt with itching, scaling, or blocked ears that no amount of cleaning seems to fix, you already know how frustrating and isolating this condition can be.
This guide walks you through everything — from what’s really happening inside and around your ear canal, to the most current medical options, to longer-term lifestyle strategies that address the root of the problem.
What Is Ear Psoriasis? An Overview
Psoriasis is a chronic autoimmune skin disease where the immune system mistakenly accelerates the skin cell lifecycle. Normally, skin cells take about 28 to 30 days to mature and shed. In psoriasis, that process compresses into just three to four days, causing a rapid buildup of cells on the skin surface.
When this process targets the ear — including the outer ear (pinna), the ear canal, and the skin behind the ear — it is called ear psoriasis, or auricular psoriasis. It is more common than most people realize; studies suggest that up to 18% of people with psoriasis experience ear involvement at some point in their lives (National Psoriasis Foundation, 2022).
Ear Psoriasis photos

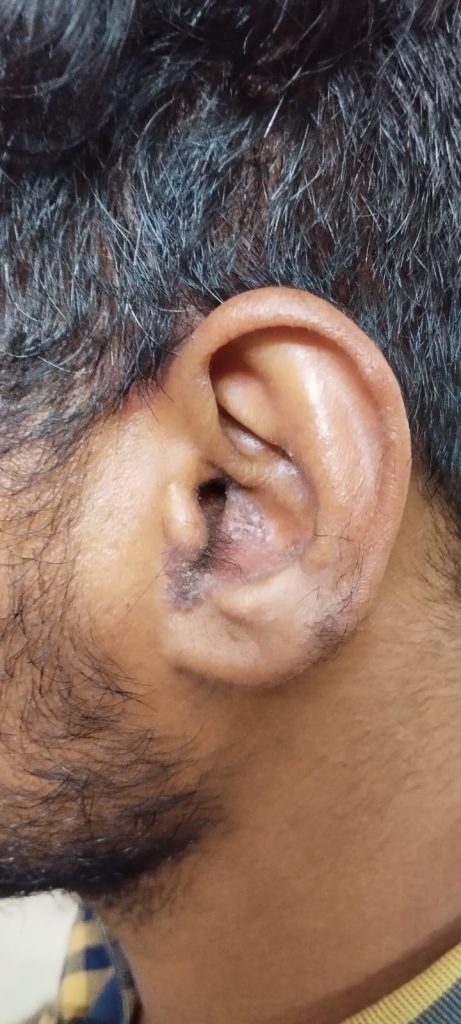
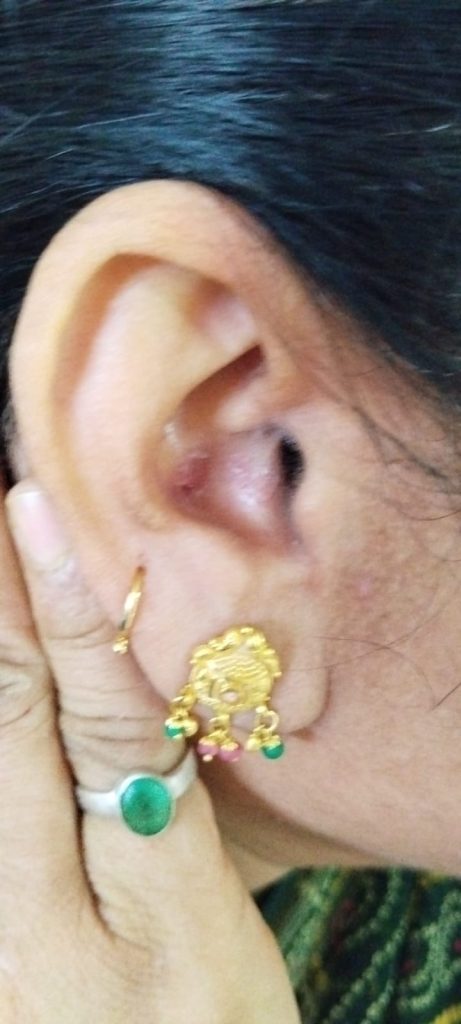
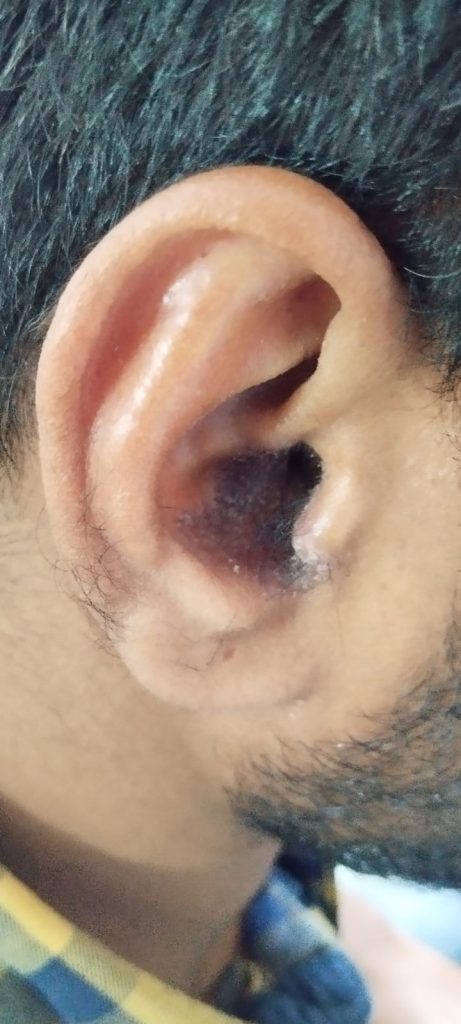
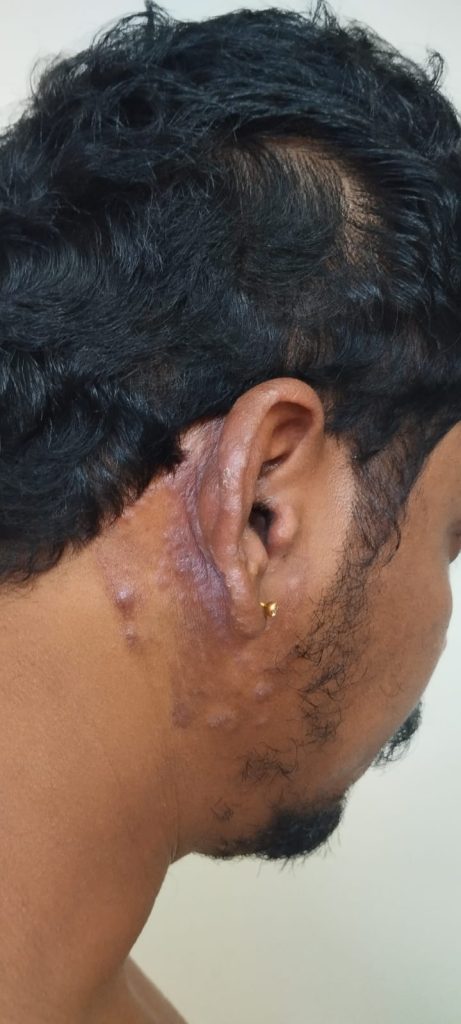
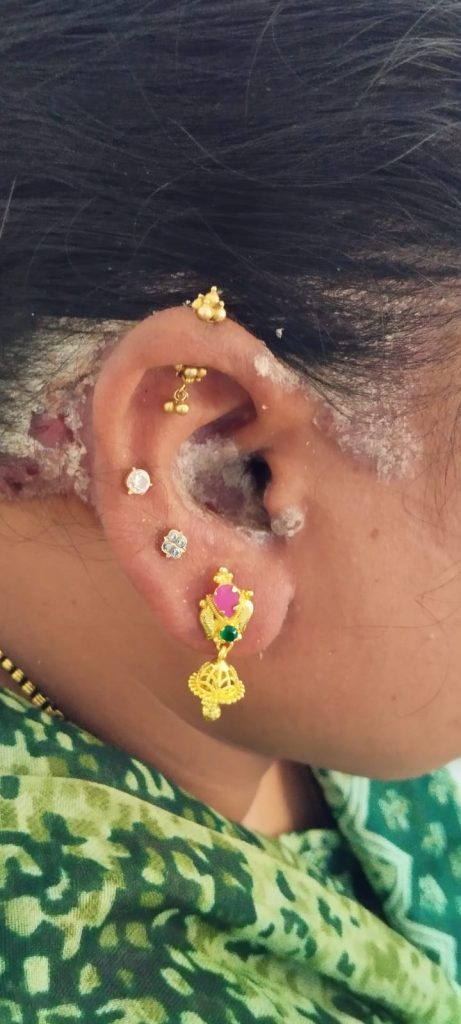
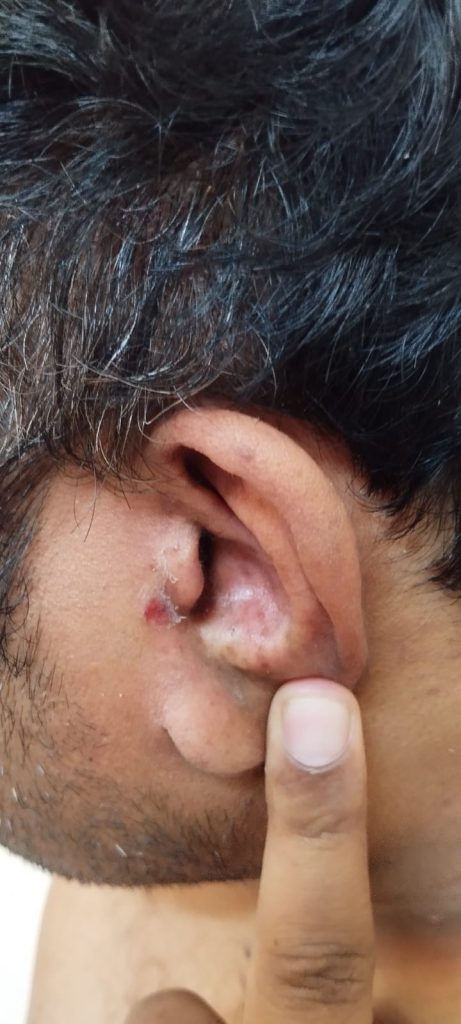
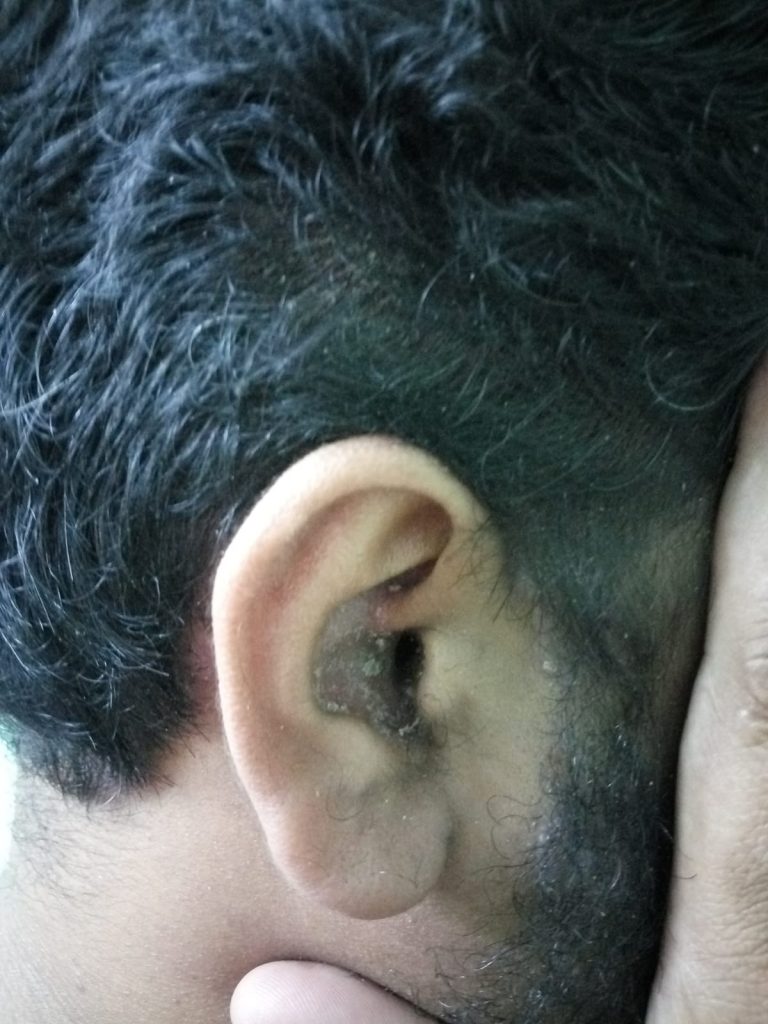
Recognizing Ear Psoriasis: Symptoms You Shouldn’t Ignore
The symptoms of ear psoriasis can range from mildly annoying to severely debilitating. What makes diagnosis tricky is that many symptoms overlap with common ear conditions like eczema, seborrheic dermatitis, or fungal infections.
Common symptoms include:
- Silvery-white or yellowish scales inside or around the ear canal
- Persistent itching, sometimes deep inside the ear
- Redness and inflammation of the outer ear and surrounding skin
- A sensation of fullness or temporary hearing loss due to scale buildup
- Dry, cracked skin behind the ears or along the ear folds
- Bleeding or cracking when scales are forcibly removed
- Tinnitus (ringing in the ears) in severe cases
The itch associated with ear psoriasis is notoriously intense. Unlike ordinary itching, it can disrupt sleep and make daily functioning difficult. Scratching brings only momentary relief and often worsens the inflammation, creating a damaging itch-scratch cycle.
What Causes Ear Psoriasis?
Psoriasis is not contagious — it cannot be passed from person to person. At its core, ear psoriasis is driven by an overactive immune response, but several factors influence why it appears or flares up in the ear region specifically.
Root causes and contributing factors:
- Genetic predisposition: About one-third of people with psoriasis have a close family member with the same condition (American Academy of Dermatology, 2023).
- Immune dysfunction: Overactivation of T-cells triggers excess production of inflammatory cytokines like TNF-alpha and interleukin-17.
- Microbiome disruption: The moist environment of the ear canal can alter the skin microbiome, making it more susceptible to flares.
- Anatomical vulnerability: The shape and enclosed nature of the ear canal make it difficult to treat topically and easier for scale to accumulate.
Common Triggers of Ear Psoriasis
Understanding what sets off a flare is essential for managing ear psoriasis long-term. Triggers vary between individuals, but some are nearly universal.
Key triggers to watch for:
- Stress — Psychological stress is the most commonly reported trigger, with research showing a clear bidirectional relationship between stress and psoriasis severity (Frontiers in Immunology, 2021).
- Infections — Streptococcal throat infections are well-known triggers, as are ear infections.
- Harsh earphones or hearing aids — Continuous pressure or moisture from devices irritates already-sensitive skin.
- Q-tip and cotton bud use — Scraping the ear canal removes the skin’s natural protective barrier and can trigger or worsen a flare.
- Cold, dry weather — Reduced humidity strips moisture from the skin.
- Alcohol and smoking — Both are independently associated with higher psoriasis severity.
- Certain medications — Beta-blockers, lithium, and antimalarials are known psoriasis aggravators.
- Dietary factors — A diet high in processed foods, sugar, and red meat can promote systemic inflammation.
How Modern Medical Science Approaches Ear Psoriasis Treatment
Conventional ear psoriasis treatment follows a staged approach — starting with the least invasive options and escalating based on severity and response. Treatment is often more challenging in the ear than elsewhere on the body due to the narrow, delicate nature of the ear canal.
Topical Treatments for Ear Psoriasis
Topical therapies are the first line of defense. Corticosteroid ear drops (such as betamethasone or fluocinolone) are most commonly prescribed to reduce inflammation and slow skin cell turnover. Vitamin D analogue creams like calcipotriol are sometimes used on the outer ear, though they are not suitable inside the ear canal.
Salicylic acid solutions are used carefully to soften and loosen scales before other treatments are applied. Tar-based preparations, while effective in some cases, are messy and carry cosmetic limitations.
Limitations of topical treatments: Long-term use of steroid drops can thin the skin, alter the ear canal’s pH, and increase the risk of secondary fungal infection. Many patients find temporary relief but experience frequent relapses.
Systemic and Biologic Treatments
For moderate to severe ear psoriasis, especially when linked to widespread plaque psoriasis, dermatologists may recommend systemic medications. Methotrexate, cyclosporine, and acitretin are older systemic options that work by suppressing the immune system globally.
Biologics — including IL-17 inhibitors (secukinumab, ixekizumab) and IL-23 inhibitors (guselkumab, risankizumab) — have revolutionized psoriasis treatment. Clinical trial data shows that many patients achieve near-complete skin clearance with these medications. However, they come with significant costs, potential long-term immunosuppression risks, and a requirement for ongoing injections or infusions.
Limitations: Biologics do not address the root cause of the disease. Once stopped, psoriasis typically returns. They also carry risks, including increased susceptibility to infections, and their safety profiles over decades are still being studied.
Procedural Interventions
In-office procedures include professional ear cleaning (microsuction or syringing) to safely remove accumulated scales. Phototherapy — specifically, narrowband UVB — has shown benefit for psoriasis but is difficult to deliver inside the ear canal.
Calcineurin inhibitors like tacrolimus ointment are sometimes used off-label for ear psoriasis, especially when steroids cannot be used long-term. Results are variable.
Why Ear Psoriasis Is Harder Than It Looks
People living with ear psoriasis often describe a level of suffering that outpaces what visible symptoms suggest to others. The combination of an invisible location, relentless itch, and social stigma makes this condition particularly hard to bear.
Physical pain points:
- Hearing loss from scale occlusion is frightening and often misdiagnosed
- Ear pain (otalgia) during flares that disrupts sleep
- Risk of secondary infections (bacterial or fungal) inside the canal
- Difficulty using earphones, hearing aids, or headsets
Psychological and quality-of-life impact: Research consistently shows that psoriasis — including in hard-to-treat areas like the ear — is associated with clinically significant rates of depression and anxiety.
A 2019 study in the Journal of the American Academy of Dermatology found that patients with psoriasis had a 39% higher risk of depression compared to those without the condition. The ear’s proximity to the brain, the chronic nature of the disease, and the itch-related sleep disruption all compound this psychological burden.
Social withdrawal is common. People with ear psoriasis often avoid social settings where they fear scales will be visible, stop using in-ear headphones, and feel self-conscious when receiving medical or grooming care.
Complications of Untreated Ear Psoriasis
Left unmanaged, ear psoriasis can lead to several complications beyond discomfort. Scale accumulation can cause a conductive hearing loss that, while usually reversible once cleared, becomes recurrent without proper management.
Secondary infections are a serious concern. The disrupted skin barrier inside the ear makes it an ideal environment for bacterial (particularly Pseudomonas aeruginosa and Staphylococcus aureus) and fungal pathogens. Chronic ear infections, if untreated, can cause scarring of the ear canal (stenosis), a condition that may require surgical intervention in severe cases.
Managing Ear Psoriasis: Day-to-Day Strategies That Make a Real Difference
Effective ear psoriasis management isn’t just about prescription medications. Daily habits form the backbone of long-term control.
Practical management tips:
- Never insert cotton buds or scratch inside the ear — use the outer ear only
- Keep the ear dry after swimming or bathing using a soft towel pat
- Use mild, fragrance-free shampoos that won’t irritate the ear canal edges
- Apply prescribed drops as directed and do not stop abruptly
- Identify and track your personal triggers using a flare diary
- Communicate openly with an ENT or dermatologist — you may need both specialists
Ayurvedic Psoriasis Diet: Foods to Eat and Avoid
Why Ayurvedic Treatment Deserves Serious Consideration for Ear Psoriasis
Modern medicine excels at controlling acute flares, but the reality is that psoriasis is a lifelong condition. Repeated reliance on steroids, immune suppressants, or biologics introduces its own risks over time. This is where Ayurveda — India’s ancient system of holistic medicine — offers something genuinely compelling.
Ayurveda does not view psoriasis as a skin disease alone. It classifies it under Kushtha, understanding it as a manifestation of disrupted metabolic and immune intelligence (Dosha imbalance), particularly Vata and Kapha. Rather than suppressing symptoms, Ayurvedic protocols aim to correct the environment in which the disease thrives.
What makes Ayurveda valuable for long-term ear psoriasis management:
- Trigger avoidance as a system — Ayurveda’s seasonal and daily routine (Dinacharya/Ritucharya) is specifically designed to minimize the environmental and lifestyle triggers that provoke autoimmune flares.
- Dietary protocols — An anti-inflammatory Ayurvedic diet (avoiding incompatible food combinations, fermented foods, and excessive nightshade vegetables) directly targets gut-skin axis dysfunction, which emerging research links to psoriasis severity.
- Panchakarma therapies — Detoxification procedures like Vamana (therapeutic emesis) and Virechana (purgation) are used to cleanse accumulated metabolic waste, potentially reducing systemic inflammation.
- Mental health integration — Yoga, Pranayama, and meditation are core to Ayurvedic treatment — and given that stress is the top psoriasis trigger, this is clinically relevant, not merely philosophical.
- Herbal formulations — Herbs like Neem, Turmeric, Manjistha, and Khadira have documented anti-inflammatory and immunomodulatory properties in peer-reviewed research.
Ayurveda is best approached not as an alternative to emergency medical care, but as a long-term parallel strategy that addresses the soil in which psoriasis grows. For ear psoriasis specifically — where conventional options are limited by anatomy — the whole-body approach of Ayurveda is particularly well-suited.
Looking for Ear Psoriasis Treatment in Bangalore, India?
If you are based in Bangalore and searching for a trusted, holistic approach to managing ear psoriasis, help is closer than you think. Visit the Psoriasis Treatment Center Bangalore for specialized Ayurvedic psoriasis treatment that goes beyond symptom suppression — addressing your diet, lifestyle, triggers, and mental well-being as a whole. With a team experienced in treating complex and chronic psoriasis cases, including difficult areas like the ear canal, the center offers personalized Panchakarma therapies, herbal formulations, and long-term management plans tailored to your body type and condition severity. If conventional treatments have left you cycling through flares without real relief, Ayurvedic care in Bangalore may be the sustainable answer you have been looking for.
Read Ayurvedic Treatment for Psoriasis: A Beginner’s Guide
Frequently Asked Questions About Ear Psoriasis Treatment
1. Can ear psoriasis go away on its own?
Psoriasis is a chronic autoimmune condition, meaning it rarely resolves permanently without intervention. Many people do experience periods of remission, but flares typically recur without addressing underlying triggers and systemic imbalance.
2. Is ear psoriasis contagious?
No. Psoriasis is an autoimmune disease — it is completely non-contagious and cannot be spread through contact, sharing items, or proximity.
3. Can ear psoriasis cause permanent hearing loss?
Typically, the hearing loss associated with ear psoriasis is conductive and temporary — caused by scale buildup blocking the canal. However, repeated secondary infections or severe, long-term inflammation can potentially cause lasting damage. Prompt management is important.
4. What is the best ear psoriasis treatment at home?
Keeping the ear clean and dry, avoiding ear canal scratching, using prescribed emollients on the outer ear, and managing known triggers (stress, diet, sleep) form the foundation of home care. Never attempt to remove inner ear scales yourself.
5. How is ear psoriasis diagnosed?
Diagnosis is clinical — a dermatologist or ENT examines the affected area. In ambiguous cases, a skin biopsy may confirm psoriasis versus seborrheic dermatitis or eczema.
6. Can I use steroid ear drops indefinitely?
No. Long-term steroid ear drops can thin the ear canal skin, increase infection risk, and cause other side effects. Your doctor should supervise the duration and transition to maintenance strategies.
7. Does diet affect ear psoriasis?
Growing evidence supports a gut-skin axis — meaning gut inflammation can worsen psoriasis. Anti-inflammatory diets (Mediterranean-style or Ayurvedic dietary protocols) appear to help some patients reduce flare frequency and severity.
8. Can stress really trigger ear psoriasis?
Yes — stress is one of the most well-documented psoriasis triggers. It activates cortisol and inflammatory neuropeptides that directly aggravate psoriatic plaques. Mind-body practices like meditation and yoga have measurable benefit.
9. Is Ayurvedic treatment safe alongside conventional ear psoriasis treatment?
In most cases, yes — but always consult both your dermatologist/ENT and your Ayurvedic practitioner before combining approaches. Some herbal formulations can interact with medications or affect liver function.
10. How long does ear psoriasis treatment take to show results?
Topical treatments may show initial improvement within two to four weeks. Systemic or biologic treatments can take two to three months for full effect. Ayurvedic protocols typically require three to six months of consistent adherence for meaningful and sustained results.
Sources and References
- National Psoriasis Foundation. (2022). Psoriasis Statistics. www.psoriasis.org
- American Academy of Dermatology Association. (2023). Psoriasis: Diagnosis and Treatment. www.aad.org
- Kamiya, K., et al. (2019). “Risk Factors for the Development of Psoriasis.” International Journal of Molecular Sciences, 20(18), 4347.
- Liang, S.E., et al. (2021). “Association Between Stress and Psoriasis Flares.” Frontiers in Immunology, 12, 662079.
- Dowlatshahi, E.A., et al. (2014). “Prevalence and Management of Ear Psoriasis.” JAMA Dermatology, 150(11), 1170–1177.
- Pona, A., et al. (2019). “Psoriasis and Depression: Shared Inflammatory Pathways.” Journal of the American Academy of Dermatology, 81(1), 31-41.
- Takeshita, J., et al. (2017). “Psoriasis and Comorbid Diseases: Epidemiology.” Journal of the American Academy of Dermatology, 76(3), 377–390.
- Charaka Samhita (classical Ayurvedic text) — Referenced via: Priya, V.K. (2014). Kushtha Chikitsa in Ayurveda. Journal of Ayurveda and Integrative Medicine.
- Mamgain, R.K., et al. (2021). “Phytochemicals in Psoriasis Management: A Review of Neem, Turmeric, and Manjistha.” Journal of Ethnopharmacology, 268.
- World Psoriasis Day Consortium. (2022). Global Report on Psoriasis. World Health Organization.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified dermatologist, ENT specialist, or Ayurvedic practitioner before making changes to your treatment plan.

